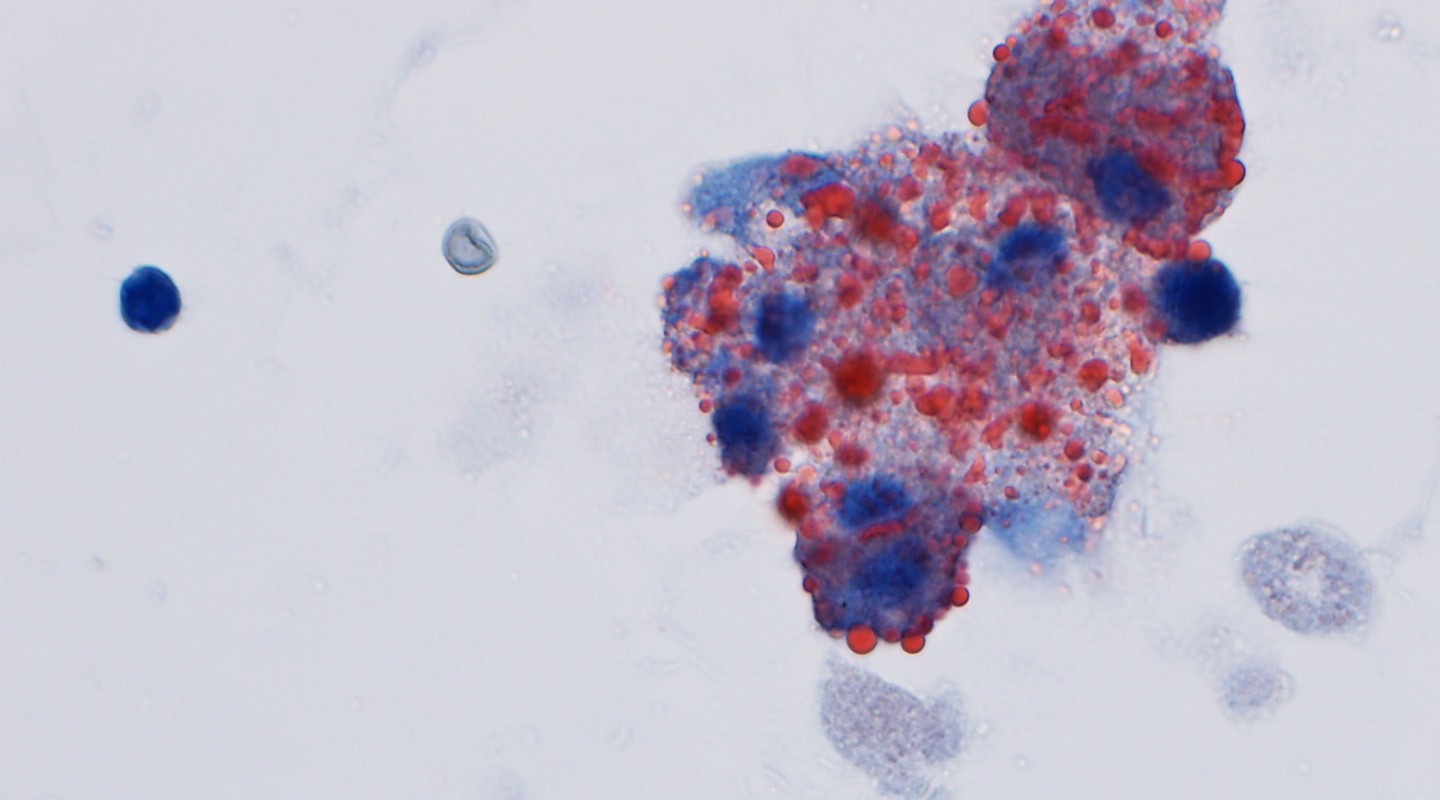
In the realm of medical diagnostics, particularly within laboratory medicine, the accuracy and reliability of results are paramount. This is especially true in cytology, a branch of pathology focused on examining individual cells to detect diseases such as cancer. Standardized cytology practices play a vital role in ensuring diagnostic accuracy and minimizing ambiguity, particularly when dealing with challenging cytology specimens. Our commitment to rigorous cytology standards significantly enhances patient care by providing cytopathologists with clear guidelines for interpreting cytologic diagnoses, ultimately leading to more effective treatment strategies.
Cytology: An Overview
Definition and Importance of Cytology
Cytology, derived from the Greek words “kytos” (cell) and “logia” (study), is the branch of pathology that deals with the microscopic examination of cells obtained from various body sites. The importance of cytology lies in its ability to detect abnormalities, such as malignancy or infection, at an early stage. Cytologic analysis plays a crucial role in diagnostic pathology, guiding clinical decisions and contributing significantly to patient care.
The Role of Cytopathology in Diagnosis
Cytopathology is a specialized area within cytology focusing on the diagnostic interpretation of cells to identify diseases. Cytopathologists examine cytology samples, including liquid-based preparations and smears, to detect neoplastic and non-neoplastic conditions. The role of cytopathology extends beyond identifying malignancy; it also aids in diagnosing infections, inflammatory conditions, and other cellular abnormalities, ensuring accurate and timely intervention.
Current Trends in Cytology Standards
Current practice in cytology emphasizes the importance of standardized reporting systems, such as the Bethesda system for reporting cervical cytology and the Paris system for reporting urinary cytology. These systems provide a structured approach to cytologic diagnoses, reducing variability and improving communication among cytopathologists and other healthcare professionals. The American Society of Cytopathology and the Papanicolaou Society of Cytopathology actively promote these standardized systems and the integration of molecular testing in cytology to enhance diagnostic accuracy.
Understanding Cytology Specimens
Types of Cytology Specimens
Cytology specimens encompass a wide range of sample types obtained through various methods, including exfoliative cytology (e.g., Pap test), aspiration cytology (e.g., fine needle aspiration of a tumor), and fluid cytology (e.g., urine cytology). Each type of specimen presents unique challenges and requires specific specimen collection and specimen processing techniques to ensure optimal diagnostic quality. These specimens are crucial for assessing lesions and detecting cellular abnormalities.
Specimen Processing Techniques
Effective specimen processing is critical to ensure the quality and diagnostic utility of cytology specimens. Techniques include fixation, staining (such as Papanicolaou stain), and slide preparation. Liquid-based cytology is increasingly used, offering advantages such as improved cell preservation and the ability to perform ancillary studies, including molecular testing, on the same sample. Proper specimen processing enhances the morphologic assessment of cells.
Challenges with Small Biopsy Specimens
Small biopsy specimens present significant challenges in cytopathology. The limited amount of tissue available may hinder comprehensive morphologic evaluation and limit the ability to perform ancillary testing. Ambiguous terminology in reporting small biopsies can lead to diagnostic uncertainty and impact patient management. Cytopathologists must employ meticulous techniques and, when necessary, utilize ancillary studies to maximize diagnostic accuracy in these challenging cases, including careful classification of any identified carcinoma.
Frequently Asked Questions
What is the primary goal of cytology?
The primary goal of cytology is to examine individual cells to detect diseases such as cancer, infections, and other abnormalities. It plays a crucial role in early diagnosis and patient care, guiding clinical decisions and treatment strategies.
How does liquid-based cytology improve diagnostic accuracy?
Liquid-based cytology improves diagnostic accuracy by providing better cell preservation, reducing obscuring factors, and allowing for ancillary testing on the same sample. This method enhances the morphologic assessment of cells, leading to more reliable cytologic diagnoses.
What is the significance of standardized reporting systems in cytology?
Standardized reporting systems, such as the Bethesda and Paris systems, provide a structured approach to cytologic diagnoses, reducing variability and improving communication among cytopathologists. These systems ensure consistent and accurate reporting, ultimately enhancing patient care.
Why are small biopsy specimens particularly challenging in cytology?
Small biopsy specimens are challenging due to the limited amount of tissue available, which can hinder comprehensive morphologic evaluation and limit the ability to perform ancillary testing. This can lead to diagnostic uncertainty and impact patient management.
How do ancillary studies contribute to cytology diagnoses?
Ancillary studies, including molecular testing and immunohistochemistry, provide additional information that complements morphologic evaluation. These studies can help confirm diagnoses, classify neoplasms, and guide treatment decisions, particularly in challenging cases.
What role do professional societies play in advancing cytology standards?
Professional societies such as the American Society of Cytopathology and the Papanicolaou Society of Cytopathology actively promote standardized systems, provide educational resources, and foster collaboration among cytopathologists. They play a critical role in advancing cytology standards and improving diagnostic accuracy.
Minimizing Ambiguity in Specimen Classification
Ambiguous Terminology in Pathology
In pathology, ambiguous terminology can significantly hinder accurate specimen classification. Cytopathologists often face challenges when interpreting reports with vague or imprecise language, leading to potential misdiagnoses. The lack of standardized terms can create variability in how lesions are classified, impacting patient care. The American Society of Cytopathology is actively working to reduce ambiguous terminology through task force initiatives and guidelines. Clear and consistent language is crucial for minimizing diagnostic errors in both surgical pathology and cytology.
The Bethesda System for Thyroid Cytology
The Bethesda System for reporting thyroid cytology is a prime example of standardized classification aimed at reducing ambiguity. This system provides clear diagnostic categories for thyroid cytology specimens, such as “benign,” “suspicious for malignancy,” or “malignant.” By using a consistent terminology, cytopathologists can communicate findings more effectively, leading to better clinical management of thyroid lesions. The Bethesda system also incorporates the results of ancillary studies, such as molecular testing, to refine diagnostic accuracy and guide treatment decisions.
Impact of Ancillary Studies in Classification
Ancillary studies, including molecular testing and immunohistochemistry, play a crucial role in refining specimen classification. In cases where morphologic features are ambiguous, these studies can provide additional information to help classify lesions more accurately. For example, molecular assays can detect specific genetic mutations associated with certain types of carcinoma or neoplasm, aiding in diagnostic accuracy. The integration of ancillary testing into routine cytology practice enhances the precision of cytologic diagnoses, leading to more personalized patient care.
The Role of Cytology in Precision Medicine
Cytology’s Contribution to Personalized Treatment
Cytology plays an increasingly important role in precision medicine by providing critical information for personalized treatment strategies. Cytology samples obtained through methods like fine needle aspiration cytology and liquid-based cytology can undergo molecular testing to identify specific genetic alterations within tumor cells. This information enables pathologists and oncologists to tailor treatment plans based on the unique molecular profile of the patient’s cancer, ensuring that the most effective therapies are selected. The department of pathology is fundamental in providing a personalized approach to medicine through diagnostic accuracy in specimen classification.
Case Studies in Diagnostic Accuracy
Numerous case studies highlight the impact of cytology on diagnostic accuracy and patient outcomes. For instance, urine cytology combined with molecular testing can improve the detection of urothelial carcinoma, enabling earlier intervention. Similarly, in cervical cancer screening, liquid-based cytology and the Pap test have significantly reduced the incidence of cervical cancer by identifying pre-cancerous lesions early on. These case studies underscore the value of cytology in improving patient care and driving advancements in diagnostic pathology, and the American Society of Cytology continues to play a role.
Future Directions in Cytopathology
The future of cytopathology lies in further integration of molecular testing and artificial intelligence to enhance diagnostic accuracy. Advanced molecular assays can identify even more subtle genetic changes, leading to more precise specimen classification. Artificial intelligence algorithms can assist cytopathologists in analyzing cytology samples, improving efficiency and reducing inter-observer variability. These advancements promise to revolutionize cytology practice, enabling even more personalized and effective patient care and minimize the chances for ambiguous terminology.
Frequently Asked Questions
What is the difference between cytology and histology?
Cytology and histology are both integral parts of diagnostic pathology, yet they examine tissue samples differently. Cytology involves the study of single cells or small groups of cells, often obtained from fluids or fine needle aspirations. Histology, on the other hand, examines larger tissue fragments to assess tissue architecture and cellular arrangements, providing a broader view of lesions and neoplasms. Each technique offers unique advantages in specimen classification.
How do cytology standards affect diagnostic outcomes?
Rigorous cytology standards are essential for ensuring diagnostic accuracy and improving patient care. Standardized specimen collection, specimen processing, and reporting protocols minimize variability in cytologic diagnoses. These standards guide cytopathologists in interpreting cytology samples, leading to more consistent and reliable results. The application of the Bethesda system and other standardized systems helps reduce ambiguous terminology and enhance communication within the clinical laboratory, directly impacting diagnostic outcomes.
What are the common challenges in processing cytology specimens?
Processing cytology specimens presents several challenges. Ensuring adequate cell preservation, particularly in liquid-based cytology, is crucial. The presence of blood or inflammatory cells can obscure morphologic details, making accurate assessment difficult. Small biopsy specimens pose additional challenges due to the limited amount of material available for analysis. Proper specimen processing techniques and the judicious use of ancillary studies are essential for overcoming these hurdles and maintaining diagnostic accuracy.
How does the Bethesda System improve classification?
The Bethesda system provides a standardized approach to classifying cytology specimens, primarily for cervical and thyroid cytology. By defining specific diagnostic categories and criteria, the Bethesda system reduces inter-observer variability and improves communication among cytopathologists. This standardized terminology enhances the consistency of cytologic diagnoses, ensuring that patient management decisions are based on clear and reliable information. The Bethesda system is endorsed by the American Society of Cytopathology and other professional organizations.
What ancillary studies are commonly used in cytology?
Ancillary studies play a vital role in enhancing the diagnostic accuracy of cytology, particularly in challenging cases. Molecular testing can identify genetic mutations associated with specific neoplasms, aiding in specimen classification and personalized treatment planning. Immunohistochemistry can help determine the cellular origin of tumors and identify specific protein markers, further refining diagnostic accuracy. These ancillary studies complement morphologic evaluation and provide valuable information for patient management, as recognized by the Papanicolaou Society of Cytopathology.